#ez-toc-container {
background: #f9f9f9;
border: 1px solid #aaa;
border-radius: 4px;
-webkit-box-shadow: 0 1px 1px rgba(0, 0, 0, .05);
box-shadow: 0 1px 1px rgba(0, 0, 0, .05);
display: table;
margin-bottom: 1em;
padding: 10px 20px 10px 10px;
position: relative;
width: auto;
}
.ez-toc-container-direction {
direction: ltr;
}
.ez-toc-list-level-1 a{
font-weight:bold;
}
Table of Contents
1. Introduction to the Connection between Heart Disease and Oral Health
Heart disease and oral health might seem unrelated at first glance, yet an increasing body of research reveals a significant connection between the two. Understanding the link between heart disease and oral health is not only a concern for healthcare professionals but also an essential topic for anyone invested in overall well-being. This introduction aims to explore these connections and underscore the importance of maintaining good oral hygiene as part of a heart-healthy lifestyle.
Exploring the Connection
The connection between heart disease and oral health is rooted in the intricate interactions within the body’s systems. Here’s an in-depth look at how these connections manifest:
-
Shared Risk Factors:
Both heart disease and poor oral health share common risk factors such as smoking, unhealthy diet, and even age. Addressing these risk factors can lead to improved heart health and better oral hygiene.
-
Inflammation as a Common Denominator:
Chronic inflammation plays a central role in both periodontal disease and cardiovascular conditions. Oral health issues might exacerbate systemic inflammation, which contributes to heart disease.
-
Bacterial Influence:
Specific bacteria that cause gum disease can enter the bloodstream and contribute to the formation of arterial plaque, leading to atherosclerosis.
The Growing Body of Research
The connection between oral and cardiovascular health continues to be validated through various scientific studies. Here’s how recent findings support this link:
-
Large-Scale Epidemiological Studies:
Investigations involving thousands of subjects have identified significant correlations between periodontal disease and the prevalence of coronary artery disease.
-
Clinical Trials:
Studies where interventions for periodontal disease resulted in improved markers for heart disease such as reduced arterial plaque and better endothelial function provide concrete evidence of the impact of oral health on heart health.
-
Case-Control Studies:
Comparative studies have noted that individuals with healthy gums generally have lower incidences of cardiovascular events than those with gum disease.
Importance of Understanding the Connection
Recognizing the connection between heart disease and oral health can greatly influence how we approach health and wellness on an individual level and within health care systems:
-
Improved Prevention Strategies:
Understanding this relationship emphasizes the necessity of regular dental check-ups as part of preventive care for heart disease.
-
Law of Unintended Benefits:
By promoting oral health, individuals unknowingly support cardiovascular health, thereby reducing the risk of a significant health burden like heart disease.
-
Patient Education:
Educating patients on the heart-oral health link can empower them to make informed decisions regarding their health practices.
Conclusion
The intersection of heart disease and oral health underscores a complex interrelation that demands attention. As awareness grows, so does the opportunity to leverage this knowledge towards healthier living. Incorporating oral health as a cornerstone of preventive care could pave the way for reducing incidences of heart disease, ultimately fostering a more holistic approach to health.
In summary, the burgeoning evidence linking oral health to heart disease should inspire proactive health measures and encourage more collaborative care between dental and medical professionals. By embracing this connection, we move a step closer to achieving comprehensive health and wellness.

2. Understanding Heart Disease: Causes and Risk Factors
Heart disease remains one of the most pervasive health challenges worldwide, affecting millions and accounting for a significant number of deaths across the globe. Understanding heart disease encompasses exploring its definitions, prevalence, and especially its multifaceted risk factors. Below is a detailed overview designed to enhance awareness and offer a nuanced understanding of this critical health issue, all while highlighting some commonly overlooked risk factors like poor oral health.
Understanding Heart Disease: Causes and Risk Factors
What is Heart Disease?
Heart disease, also known as cardiovascular disease, refers to a range of conditions that affect the heart. These include diseases of the blood vessels, such as coronary artery disease, heart rhythm problems (arrhythmias), and heart defects you’re born with (congenital heart defects), among others. Each variation of heart disease comes with its specific symptoms, and treatment, making personalized medical advice crucial.
Prevalence of Heart Disease
The prevalence of heart disease is alarming and demands immediate attention from health practitioners and individuals alike. According to the World Health Organization, cardiovascular diseases are the leading cause of death globally, claiming an estimated 17.9 million lives annually. In the United States alone, the Centers for Disease Control and Prevention reports that heart disease is the leading cause of death for men, women, and people of most races and ethnicities.
Major Risk Factors for Heart Disease
Understanding the primary risk factors is pivotal for preventive measures. The most common risk factors are:
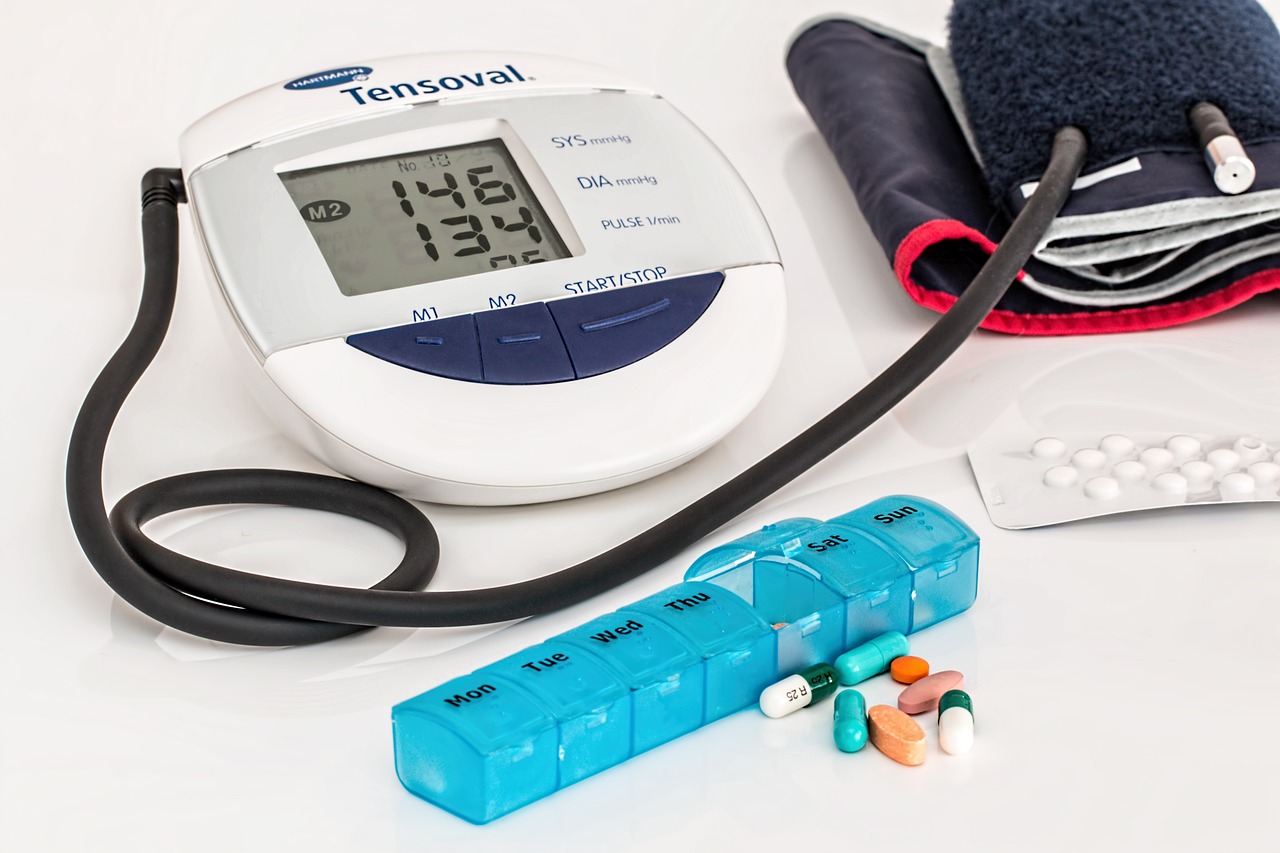
- High Blood Pressure: Often dubbed the “silent killer” due to its asymptomatic nature, high blood pressure increases the risk of heart disease significantly.
- High Cholesterol Levels: Excessive levels of bad cholesterol (LDL) can lead to plaque buildup in the arteries, impeding blood flow.
- Smoking: Smoking damages the blood vessels, leading to atherosclerosis and greater risk for heart disease.
- Diabetes: High blood sugar from diabetes can damage blood vessels and the nerves that control your heart.
- Poor Diet and Physical Inactivity: Diets high in saturated fats, salt, and sugar, coupled with lack of exercise, contribute towards obesity, hypertension, and ultimately heart disease.
- Excessive Alcohol Use: Overconsumption can lead to high blood pressure, heart failure, and even stroke.
- Genetic Factors: A family history of heart disease can increase individual risk.
Commonly Overlooked Risk Factors
While the above-listed factors are widely recognized, certain risk factors often fly under the radar. These overlooked influencers also contribute significantly towards heart disease.
- Poor Oral Health: Although surprising to many, there is a substantial link between oral health and heart disease. Inflammation caused by gum disease can contribute to heart disease as the bacteria from gum infections can enter the bloodstream and affect cardiovascular health. Proper oral hygiene, including regular brushing, flossing, and dental checkups, is therefore crucial.
- Sleep Apnea: Sleep apnea, a disorder in which breathing repeatedly stops and starts, is linked to high blood pressure, a risk factor for heart disease. Treating sleep apnea not only improves sleep quality but also may lower heart disease risk.
- Stress and Mental Health: Chronic stress, anxiety, and depression have physiological effects on the body that increase the risk of heart disease. Stress management techniques and mental health care can therefore indirectly aid in heart health.
- Loneliness and Social Isolation: Psychological and emotional stress from loneliness and social isolation can escalate the risk of heart conditions. Emotional support and connectedness are important for overall health.
- Air Pollution: Long-term exposure to polluted air can contribute to heart disease, as air pollutants can harm blood vessels that lead to plaque formation, affecting heart health.
- Excessive Sitting: With the rise in sedentary jobs and lifestyles, long durations of sitting have been linked to increased heart disease risk. Regular movement, breaking up long periods of inactivity, and engaging in physical exercise are recommended.
Conclusion
In conclusion, understanding the multifactorial nature of heart disease is essential for developing preventive strategies. While mainstream risk factors such as high blood pressure, cholesterol, and smoking are critical, recognizing overlooked elements like oral health and social factors can enhance comprehensive healthcare approaches.
By addressing both recognized and lesser-known risk factors, individuals can take proactive steps in maintaining heart health, while health practitioners can offer more tailored treatment and preventive measures. Regular health checkups, lifestyle modifications, and staying informed about heart health can collectively contribute to reducing the burden of heart disease globally.
Make heart health a priority by staying informed. Knowledge and proactive measures are key in combating this global health issue. Aim for regular health assessments, cultivate a balanced diet, ensure adequate physical activity, and maintain robust oral hygiene to optimize cardiovascular health.

3. The Science Behind Oral Health’s Impact on Heart Health
Maintaining good oral health does far more than just give you a bright smile; it plays a crucial role in ensuring optimal overall health. Research has increasingly shown a significant link between oral health and heart health. This is a fascinating area of study that reveals how oral health issues, particularly gum disease, can lead to inflammation and potentially affect the cardiovascular system. Understanding the journey of specific bacteria from the oral cavity to the bloodstream opens a window to preventive healthcare strategies.
In this segment, we will delve into the science behind oral health’s impact on heart health, explore the mechanisms at play, and identify the specific bacteria involved.
The Connection Between Oral Health and Heart Health
The mouth is a gateway to the body and a critical indicator of overall health. When oral hygiene is neglected, it can lead to gum diseases such as gingivitis and periodontitis. Periodontitis is a severe gum infection that damages soft tissue and, without intervention, can destroy the bone that supports your teeth. Beyond oral cavities, these bacteria can enter the bloodstream, affecting areas beyond the mouth.
Once in the bloodstream, harmful bacteria can cause inflammation in the blood vessels, contributing to the buildup of plaques, which can harden arteries (atherosclerosis), potentially leading to heart blockages, heart attacks, and even strokes. Health experts and researchers continue to investigate how these mechanisms affect individuals with pre-existing heart conditions and those with no recognized risk factors.
The Role of Inflammation
Inflammation is a key biological process that results from the body’s attempt to protect and heal itself after an infection, injury, or exposure to harmful substances. While inflammation can be protective, chronic inflammation can lead to various diseases, including cardiovascular diseases.
Mechanism of Inflammation in Gum Disease
- When plaque, a sticky film of bacteria, accumulates on teeth and is not removed, it can harden into tartar, leading to inflammation of the gums, known as gum disease or gingivitis.
- Unchecked gingivitis evolves into periodontitis, wherein the gums pull away from the teeth, allowing bacteria to form in these “pockets” and damage the bone supporting teeth.
- The immune system reacts to these bacterial infections, producing inflammatory markers and responses that can affect the entire body.
Link to Cardiovascular System
- The bacteria from the periodontal infection can enter the bloodstream.
- These pathogens trigger systemic inflammation and contribute to plaque formation in arteries.
- Ultimately, this increases the risk of atherosclerosis, leading to potential cardiovascular events such as heart attack or stroke.
Bacteria Responsible for Oral-Systemic Health Link
Numerous studies focus on identifying specific oral bacteria that can travel from the mouth to other parts of the body and cause systemic issues.
Specific Bacteria and Their Pathway
- Porphyromonas gingivalis: Known as a major pathogen in periodontitis, this bacterium can invade and persist within arterial cells, contributing significantly to atherosclerosis.
- Streptococcus mutans: Typically associated with tooth decay, research suggests that upon entering the bloodstream, it can adhere to damaged heart valves, potentially leading to infective endocarditis.
- Fusobacterium nucleatum: This bacterium is implicated in both periodontal disease and colorectal cancer, pointing to its versatility and ability to impact various systemic pathways.
Research is ongoing, and scientists are still unraveling the complex interactions between these bacteria and our body’s systems.
Preventive Measures and Oral Hygiene Practices
To mitigate the risk of cardiovascular issues associated with poor oral health, it is critical to practice diligent oral hygiene and visit dental professionals regularly. Below are strategies individuals can integrate into their lifestyle:
- Brush teeth at least twice daily with fluoride toothpaste to help remove plaque and prevent oral diseases.
- Floss daily to clean areas between teeth where a toothbrush can’t reach.
- Maintain a balanced diet and reduce sugar intake, which can contribute to tooth decay.
- Avoid tobacco products that can exacerbate gum diseases.
- Schedule regular dental check-ups and professional cleanings.
Beyond individual measures, better understanding and awareness at a policy and community level can amplify these preventive effects, leading to better public health outcomes.
In conclusion, the intricate link between oral and heart health underlines the importance of comprehensive healthcare approaches and lifestyle choices conducive to engaging in proactive health practices. While significant research is still necessary to fully understand all mechanisms involved, the existing data highlights a compelling reason to maintain good oral hygiene not just for your mouth but also for greater systemic advantages, including heart health.
4. Recognizing the Signs: Oral Health Problems that May Indicate Heart Health Issues
Understanding the intricate connection between oral health and heart health is essential in maintaining overall well-being. Recent studies have highlighted the potential link between oral health problems and heart health issues, making it imperative for individuals to be vigilant about the signs and symptoms that could hint at underlying cardiovascular conditions. Recognizing these signs early on through regular dental check-ups can play a crucial role in preventing heart disease. This segment will delve deeper into the various oral health symptoms that might indicate heart health concerns and emphasize the importance of proactive dental care.
Identification of Oral Health Symptoms that Could Signal Heart Health Concerns
The mouth serves as a window to the body, providing visible signs of potential internal problems, including those related to heart health. Oral health problems can sometimes reflect issues in other parts of the body, particularly the cardiovascular system. Here are some oral symptoms that may suggest heart health concerns:
-
Gum Disease (Periodontal Disease):
Periodontal disease, characterized by inflammation, bleeding, or tender gums, has been associated with an increased risk of heart disease. The bacteria causing gum infections can enter the bloodstream, potentially leading to a build-up of arterial plaque and contributing to heart conditions.
-
Chronic Bad Breath (Halitosis):
Persistent bad breath might be more than a simple hygiene issue. It can indicate an underlying infection or disease, including those related to the heart. Poor heart function can lead to reduced blood flow, resulting in an accumulation of bacteria in the mouth.
-
Loose or Shifting Teeth:
Severe gum disease can lead to the loosening of teeth, which may signal underlying inflammation—a common factor in heart disease risk.
-
Mouth Ulcers and Tooth Loss:
Frequent mouth ulcers or unexpected tooth loss can indicate systemic problems such as cardiovascular disorders. These manifestations should not be overlooked.
-
Swollen and Bleeding Gums:
The inflammation of blood vessels in swollen or bleeding gums can mirror inflammation in the cardiovascular system, which may suggest a relationship between gum health and heart health.
The Importance of Early Detection and Regular Dental Check-ups in Preventing Heart Disease
Identifying oral health issues at an early stage can significantly help in mitigating the risk of developing serious heart conditions. Here’s how prioritizing dental health contributes to heart disease prevention:
-
Regular Dental Examinations:
Frequent dental check-ups enable early detection of gum disease and other oral issues. Timely intervention can prevent the progression of gum disease, subsequently reducing the risk associated with heart health problems.
-
Professional Cleanings:
Alongside daily flossing and brushing, professional dental cleanings are critical for removing plaque and tartar build-up, which are potential contributors to gum disease and cardiovascular issues.
-
Comprehensive Health Monitoring:
During dental visits, your dentist can notice changes in your oral health that might suggest broader health conditions, including those related to heart health, encouraging a multidisciplinary approach to healthcare.
-
Patient Education:
Regular consultations with dental professionals provide an opportunity for patient education regarding the implications of oral health on overall health, fostering a deeper understanding and more effective personal healthcare practices.
-
Emphasis on Preventive Care:
Preventive dental care routines help maintain optimal oral health, indirectly supporting heart health by minimizing risks of inflammation and bacterial spread through the bloodstream.
Conclusively, while oral health alone may not directly cause heart problems, the clinical evidence suggests a close association through common risk factors such as inflammation. Therefore, recognizing the signs early and committing to regular dental check-ups can facilitate the maintenance of both oral and heart health, contributing to the prevention of heart disease. By advocating for a comprehensive approach to health, individuals are empowered to take proactive steps in mitigating potential risks and enhancing their overall well-being.