#ez-toc-container {
background: #f9f9f9;
border: 1px solid #aaa;
border-radius: 4px;
-webkit-box-shadow: 0 1px 1px rgba(0, 0, 0, .05);
box-shadow: 0 1px 1px rgba(0, 0, 0, .05);
display: table;
margin-bottom: 1em;
padding: 10px 20px 10px 10px;
position: relative;
width: auto;
}
.ez-toc-container-direction {
direction: ltr;
}
.ez-toc-list-level-1 a{
font-weight:bold;
}
Table of Contents
1. Introduction to the Relationship Between Gum Disease and Arthritis
Gum disease, also known as periodontal disease, is a pervasive oral health issue that affects millions of people worldwide. It is characterized by inflammation, bleeding, and infection of the gums, which can eventually lead to tooth loss if left untreated. This condition is primarily caused by the build-up of plaque – a sticky film of bacteria that forms on the teeth. Despite regular dental hygiene practices, gum disease remains a prevalent issue, affecting nearly 47.2% of adults over 30 in the United States alone.
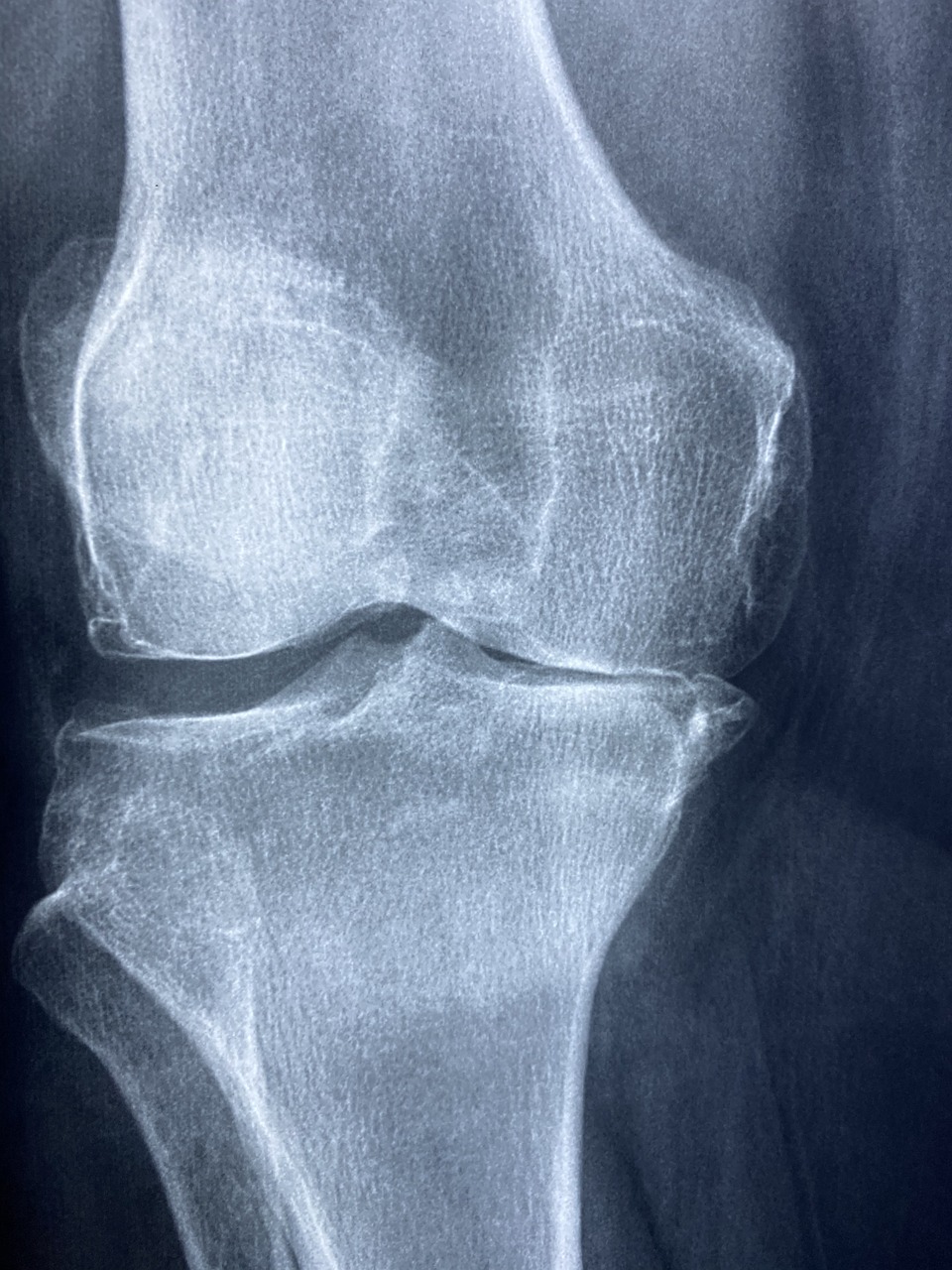
On the other hand, arthritis is another widespread health concern, particularly affecting the elderly population. It encompasses a range of conditions characterized by inflammation, pain, and stiffness in the joints. There are several different types of arthritis, each with its own unique manifestations and challenges:
- Osteoarthritis: The most common form, often described as a degenerative joint disease, which occurs when the cartilage that cushions the ends of bones gradually wears away.
- Rheumatoid Arthritis: An autoimmune disorder where the body’s immune system attacks the joints, leading to swelling and pain.
- Psoriatic Arthritis: Associated with the skin condition psoriasis, this type involves joint inflammation accompanied by skin lesions.
- Gout: Known for causing sudden, severe episodes of pain and swelling, commonly in the big toe.
Arthritis symptoms can greatly affect the quality of life, leading to decreased mobility and function. Common symptoms include:
- Joint Pain: A primary and persistent symptom that can range from mild to severe.
- Stiffness: Particularly noticeable in the morning or after sitting for long periods.
- Swelling: Inflammation that can cause visible swell in the affected areas.
- Reduced Range of Motion: Difficulty in moving the joints freely.
Recent studies have explored the hypothesis of a potential link between gum disease and arthritis. This burgeoning area of research suggests that the inflammation prevalent in gum disease may share a relationship with inflammation in arthritis, implying that oral health could have a systemic impact.
Researchers postulate that chronic inflammation could be a common denominator, potentially triggering or exacerbating arthritis symptoms. The bacteria responsible for periodontal disease may enter the bloodstream, stimulating an inflammatory response elsewhere in the body, including the joints.
The hypothesis suggests:
- Systemic Inflammation: Gum disease may increase systemic levels of inflammation, contributing to the development or worsening of arthritis.
- Shared Risk Factors: Both conditions share risk factors such as smoking and obesity, which may exacerbate their co-occurrence.
- Immune Mechanism: An autoimmune response prompted by oral bacteria could influence joint health, particularly in autoimmune forms like rheumatoid arthritis.
This potential correlation between gum disease and arthritis underscores the importance of holistic health approaches, emphasizing that maintaining oral health could be significant not just for dental well-being but also for overall physical health. Understanding the connection between dental hygiene and joint health might pave the way for novel preventative strategies and therapeutic interventions.

2. Scientific Evidence Supporting the Connection
Scientific research has increasingly drawn connections between different diseases, offering insights that go beyond surface-level symptoms. The link between gum disease and arthritis, specifically rheumatoid arthritis, stands as a prime example of this interconnectedness. Here, we summarize key studies and research findings, explore the role of bacteria like Porphyromonas gingivalis in both conditions, and explain the shared inflammatory response present in both gum disease and arthritis.
Summarizing Key Studies and Research Findings
Over the past few decades, numerous studies have delved into the relationship between periodontal disease and arthritis. Researchers have identified a bidirectional link, suggesting that inflammation in one condition may influence the other. The evidence supporting this connection is compelling:
- Epidemiological Studies: A significant number of epidemiological studies have reported a higher prevalence of periodontal disease in patients with rheumatoid arthritis compared to the general population. Such studies underscore a possible association between the two diseases.
- Clinical Trials: Clinical trials show that treating periodontal disease can help alleviate symptoms of arthritis. For example, patients receiving periodontal therapy often experience reduced joint pain and swelling.
- Genetic Research: Genetic studies reveal that certain genetic predispositions may increase the risk for both periodontal disease and rheumatoid arthritis. These findings suggest a common genetic basis for these inflammatory conditions.
The Role of Bacteria Like Porphyromonas Gingivalis
A significant breakthrough in understanding the link between gum disease and arthritis came with the identification of Porphyromonas gingivalis (P. gingivalis), a bacterium commonly found in chronic periodontitis. Research indicates that this bacterium might play a critical role in the pathogenesis of both periodontal disease and rheumatoid arthritis.
- Enzymatic Action: P. gingivalis produces enzymes called gingipains, which can modify proteins in a way similar to citrullination—a process implicated in the autoimmune response in rheumatoid arthritis.
- Immune System Interaction: The bacterium can disrupt the immune system, enhancing the body’s inflammatory response. This disruption is seen in the excessive inflammation associated with both gum disease and rheumatoid arthritis.
- Mimicry and Autoimmunity: Molecular mimicry induced by P. gingivalis may lead to the formation of autoantibodies found in rheumatoid arthritis, such as anti-citrullinated protein antibodies (ACPAs).
Explaining the Inflammatory Response Common to Both Conditions
Inflammation is the body’s natural response to infection or injury, but chronic inflammation can lead to tissue damage and contribute to the development of diseases such as gum disease and arthritis. Here’s how the inflammatory response is common to both:
- Chronic Inflammation: Both conditions involve chronic inflammation, which can progress over time if untreated. This persistent inflammation can result in the destruction of gum tissues in periodontal disease and joint tissues in arthritis.
- Increased Cytokines: Studies have noted elevated levels of pro-inflammatory cytokines like TNF-alpha and IL-1 in both diseases. These cytokines are pivotal in mediating inflammation and tissue damage.
- Systemic Link: The inflammatory mediators from periodontal disease can enter the bloodstream, potentially worsening systemic inflammation and thereby exacerbating arthritis.
In conclusion, the scientific evidence strongly supports a connection between gum disease and arthritis. Through further research, understanding these links may pave the way for better diagnostic tools and therapeutic strategies that address both conditions simultaneously.

3. Biological Mechanisms Linking Gum Disease and Arthritis
When delving into the intricate connection between gum disease and arthritis, it is pivotal to comprehend the biological mechanisms that interlink these two seemingly disparate conditions. Recent studies have highlighted shared inflammatory pathways, shed light on the impact of periodontal disease on systemic inflammation, and underscored the critical roles of immune system responses and autoimmunity.
Inflammatory Pathways Involved in Both Conditions
Inflammation is a common thread that ties gum disease and arthritis together. Understanding the inflammatory pathways involved offers insights into their interconnectedness.
- Pro-inflammatory Cytokines: Both conditions are marked by elevated levels of pro-inflammatory cytokines. In gum disease, bacteria such as Porphyromonas gingivalis trigger the production of cytokines like TNF-α, IL-1, and IL-6. Similarly, these cytokines are prevalent in arthritic joints, driving inflammation and joint destruction.
- Toll-like Receptors (TLRs): TLRs play a crucial role in the innate immune response by recognizing microbial invaders and activating immune pathways. In periodontal disease, bacterial components activate TLRs, which may translate into systemic inflammatory responses contributing to arthritis.
- Nuclear Factor-kappa B (NF-kB) Pathway: This pathway is pivotal in regulating the immune response to infection. Both gum disease and arthritis involve the activation of NF-kB, which controls the expression of inflammatory genes, ramping up the inflammation observed in both conditions.
The Impact of Periodontal Disease on Systemic Inflammation
Periodontal disease has been increasingly recognized as a significant contributor to systemic inflammation, potentially exacerbating conditions such as arthritis.
- Entry of Pathogens into the Systemic Circulation: Periodontal disease allows oral bacteria to enter the bloodstream, which can lead to chronic systemic inflammation. This systemic invasion by oral pathogens is associated with an increased inflammatory burden on distant sites, including joints.
- Systemic Inflammatory Response: The body’s response to periodontal pathogens includes an elevated systemic inflammatory response, characterized by increased levels of circulating inflammatory mediators. These mediators can exacerbate the inflammatory milieu in arthritic joints.
- Acute-Phase Proteins: Periodontal infections drive the production of acute-phase proteins like C-reactive protein (CRP) and fibrinogen, which are markers of systemic inflammation. Elevated levels of these proteins correlate with increased arthritis symptoms and progression.
The Significance of Immune System Responses and Autoimmunity
The immune system’s response to persistent inflammation in periodontal disease may inadvertently contribute to autoimmune processes seen in arthritis.
- Autoimmune Cross-Reactivity: Chronic exposure to periodontal pathogens may provoke the immune system to produce antibodies that cross-react with host tissues, a process suspected in the pathogenesis of rheumatoid arthritis. This cross-reactivity can lead to the destruction of joint tissues.
- Adaptive Immunity Dysregulation: The persistent inflammatory environment in periodontal disease can lead to the dysregulation of adaptive immunity. This dysregulation may promote autoimmunity by altering the balance between T regulatory cells and Th17 cells, crucial players in both gum disease and arthritis.
- B-Cell Activation and Autoantibody Production: Periodontal disease can aberrantly activate B-cells, leading to the production of autoantibodies that target joint components. These autoantibodies are significant in rheumatoid arthritis and contribute to chronic joint inflammation and damage.
In conclusion, understanding the intricate pathways linking gum disease and arthritis helps in recognizing the possibility of intervening in these pathways to alleviate symptoms and potentially alter the course of both conditions. The inflammatory pathways shared between these conditions, the impact of periodontal disease on systemic inflammation, and the role of immune responses and autoimmunity underscore the complex interplay between oral health and systemic diseases.
4. Preventive Measures and Treatment Strategies
Arthritis, a condition characterized by inflammation and pain in the joints, affects millions of people worldwide. While there are multiple factors contributing to its onset and progression, emerging research suggests that oral hygiene may play a crucial role in potentially mitigating arthritis symptoms. In this segment, we will explore the significance of maintaining excellent oral hygiene in managing arthritis, as well as an overview of current treatment strategies and innovations targeting both oral health and joint issues. Additionally, we will discuss impactful lifestyle changes and dietary recommendations that support overall oral and joint health.
Importance of Oral Hygiene in Potentially Mitigating Arthritis Symptoms
Maintaining optimal oral hygiene is paramount not only for preventing dental issues but also for potentially mitigating symptoms of arthritis. There is a growing body of evidence linking periodontal disease — a chronic inflammatory condition affecting the gums — with an increased risk of rheumatoid arthritis. One hypothesis is that bacteria from oral infections can trigger or worsen the inflammatory processes associated with arthritis.
- Reduction of Inflammation: Regular brushing, flossing, and professional dental cleanings help to reduce plaque buildup and inflammation in the gums. This reduction in oral inflammation may subsequently help in lowering systemic inflammation, which is a hallmark of arthritis.
- Prevention of Bacterial Spread: Good oral hygiene practices limit the proliferation of harmful bacteria in the mouth, thus preventing bacteria from entering the bloodstream and potentially affecting the joints.
- Improved Immune Response: A healthy oral cavity can support a better-functioning immune system, which is crucial for individuals with autoimmune conditions like rheumatoid arthritis.</